-

-

-
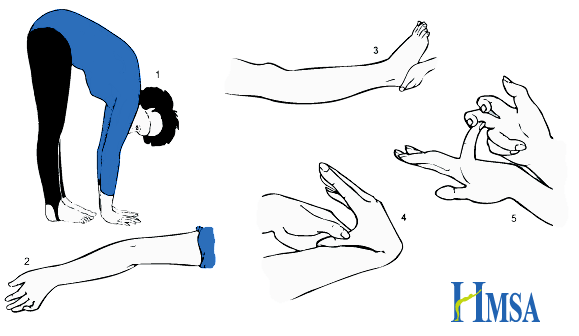
Each of these movements are signs of hyper-mobility. Image: hypermobility.org
-

-

We’re often told that flexibility is good for cyclists – tight muscles can pull on weaker muscles and create discomfort. However, flexibility and mobility are two different things, and riders struggling with hypermobility will quickly tell you that it’s not so beneficial.
We asked Osteopath Jill Shooter to explain the difference between flexibility, and hyper-mobility – and how the latter can affect cyclists….
What is hypermobility?
As an osteopath working with athletes I often hear: “oh, I have been told I am hyper-mobile!” This is useful as I can then target my treatment. However I find there is some confusion as to what being hyper-mobile actually means.
Simply put, Hyper, means over, above, excessive. Mobility, means movement. Add them together and you get excessive movement.
Hyper-mobility and hyper-flexibility are often mixed up. An individual you can be very flexible without being hyper-mobile.
Static or Dynamic Stretches: Which are Best for Cyclists?
Flexibility is the ability to bend, as seen in many yoga poses, ballet dancers and gymnasts. This is usually through the pliability of muscles and their ability to stretch. Some people find it easy to reach to the floor with the knee in a normal straight position, others not so.
Mobility relates more to the joints of the body and specifically the ligaments which surround them and support them.
Ligaments can be described as the joint’s seat belt or guide ropes. They work to restrain the joint and keep it aligned within range of movement, allowing the joint to function and the body to move safely and without pain.




